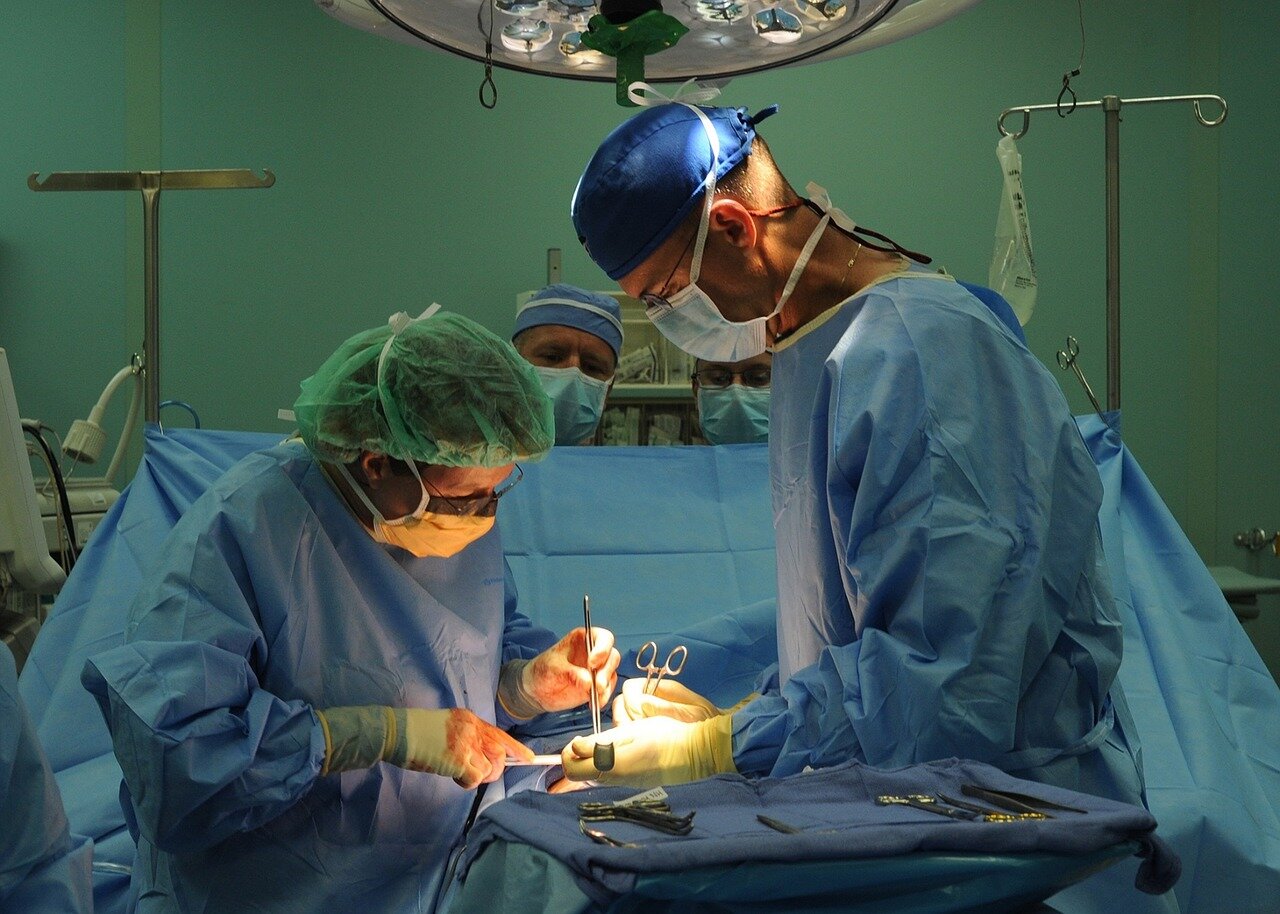
Last month, the New York Times ran a cautionary tale about the heart surgery and care astronaut Neil Armstrong received and his death two weeks later at a community hospital in a Cincinnati suburb in 2012.
The Times had received documents from an anonymous tipster who said he/she was “compelled to share this information” so “others can be saved as a result of the dissemination of this information to the public because this American hero did not have to die an untimely death.”
The hospital had made a secret $6 million settlement with the family, the Times reported, and consulted cardiac experts who pointed out numerous trouble spots in Armstrong’s care. One of those experts Dr. Ashish Jha, a professor of medicine at Harvard University, told the paper, “It feels to me like his death was wholly preventable. It’s not completely clear to me he needed the cardiac surgery that he got.”
The Times noted that the records did not say why Armstrong or his family chose a community hospital rather than the University of Cincinnati Medical Center, a larger academic institution that perhaps had more experience dealing with patients like Armstrong.
That’s the takeaway for countless others considering surgeries and procedures, especially ones that are complex. You want your surgeries done at facilities by surgeons who have experience and expertise at doing them.
Shortly before the Times published its stories, a Washington-based organization, The Leapfrog Group, released a report on minimum volume requirements for eight high-risk procedures.
Leapfrog is one of many organizations that make public information about hospital safety. I believe it is one of the most credible. Its warnings about hospitals performing too few complicated procedures that carry a high risk of complications, even death, are to be taken seriously.
Now Leapfrog has a new standard that sets minimum targets that both hospitals and individual surgeons should meet for patient safety. Previously they had standards only for hospitals.
“Studies that have looked at correlation show you have a greater risk of dying when you’re at a lower volume hospital,” says Leah Binder, who heads the group.
Her group does not believe it is safe for patients if their surgeons have not done a minimum number of eight complicated procedures. Those are surgeries, she said, where compelling evidence shows that volume is crucial to positive outcomes.
The procedures are: bariatric surgery for weight loss; carotid endarterectomy; esophageal resection for cancer; lung resection for cancer; mitral valve repair and replacement; open abdominal aortic aneurysm repair; pancreatic resection; and rectal cancer surgery.
For example, for a cancer lung resection, only about 22 percent of hospitals and 17 percent of surgeons met Leapfrog’s standard for adequate experience with these procedures. Bariatric surgeries for weight loss had the best numbers, with about 68 percent of hospitals meeting the standard and 51.5 percent of the surgeons doing the same.
I asked Binder why bariatric surgeries had the best results. She explained that health insurers have imposed regulations for covering the procedure, and they may require preauthorization and other checks. “Because of that scrutiny, we think they are better.”
In other words, insurance company oversight may be a good thing, especially since three-quarters of hospitals overall had not established criteria to determine whether the other seven procedures on Leapfrog’s list were appropriate for the patient.
Binder said that rural hospitals were most likely to fall short of the volume requirements. They struggle because sparse populations in their areas mean they don’t perform the same procedure often enough to gain expertise.
“The priority has to be not the hospital but the people served by their hospital.”
Patients must understand the level of risk they face if they choose to have complicated procedures done at a hospital with such low volume.
“Some people may not want to drive to a facility that’s further away, but at least they should understand that the procedure is not that safe,” Binder warns.
The hospital industry maintains that attributing surgical expertise only to the numbers of procedures performed ignores other safety improvement strategies.
Binder says she can’t say performing 100 surgeries is better than 90, but “I do know that 100 is better than one, two, or three. “People in health care know it, and it’s time the rest of the people know that, too.”
What’s been your experience with hospitals or surgeons harming a loved one? Write to Trudy at [email protected].
This piece was originally published as part of Rural Health News Service series, “Thinking About Health,” on Aug. 13, 2019.